Your Honest Guide to Recovery

The Ultimate Athlete's Guide
From epic game-winning moments to unexpected injuries, every athlete faces the challenge of bouncing back. Let’s break down the most common sports injuries and how to come back stronger than ever!
Injuries featured: ACL Tear, Fractures, Concussions, and Meniscus tears.
ACL Tear
(Anterior Cruciate Ligament)
What is It?
An ACL injury refers to a tear or sprain of the anterior cruciate ligament (ACL), a tough band of tissue that connects the thigh bone (femur) to the shinbone (tibia).
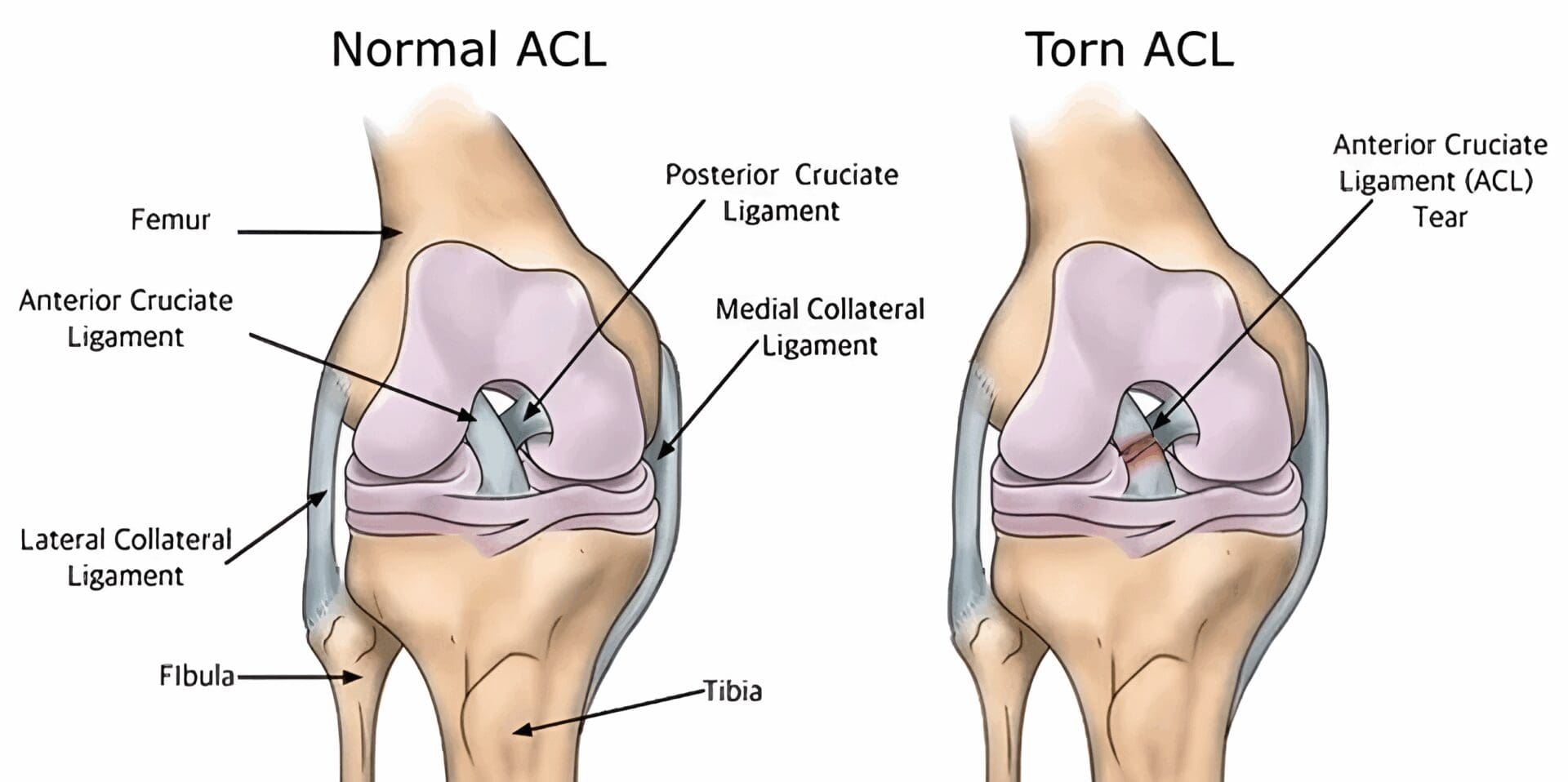
Signs of a Potential ACL Tear
When a potential ACL tear occurs, there are several key signs and symptoms to be aware of. Many individuals report hearing or feeling a loud popping sound in their knee at the time of injury. This is often accompanied by severe pain, making it difficult to continue any activity.
Elaboration of Symptoms
Important Note
These symptoms can also be present with other types of knee injuries. It's crucial to seek a professional medical evaluation for a proper diagnosis and treatment plan.
How ACL Tears Occur
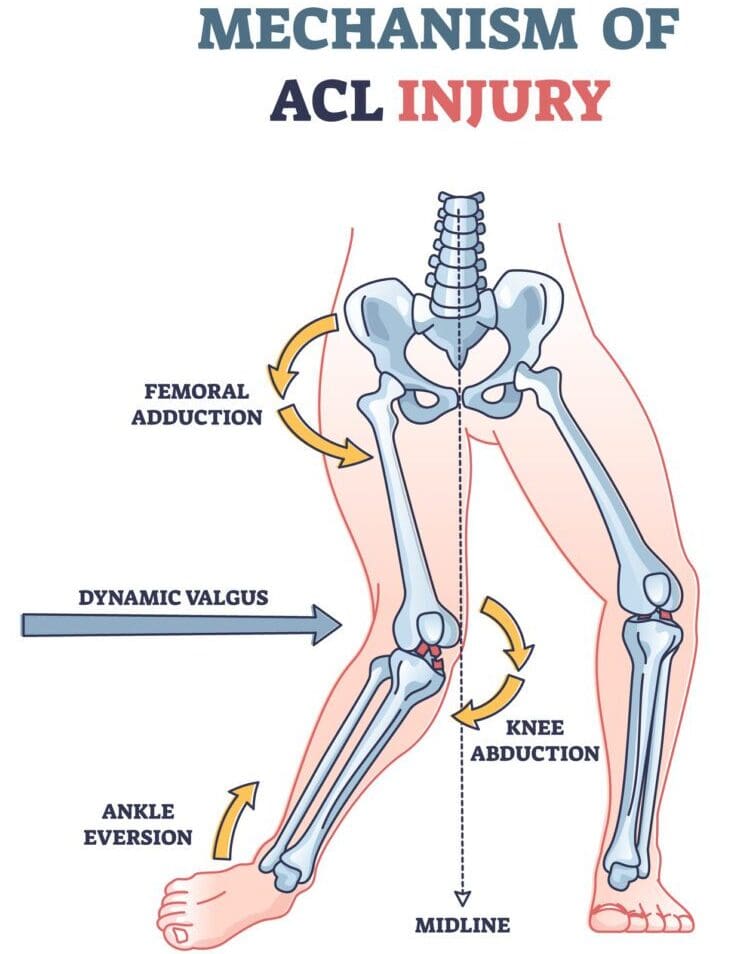
ACL tears often happen due to sudden twisting movements or a direct impact to the knee, particularly during sports activities. The tear occurs when the knee is forced beyond its normal range of motion, causing the ACL to stretch or tear. Common scenarios include:
Elaboration
Mechanism of Injury
The ACL is a strong ligament that stabilizes the knee joint. It is injured when excessive force is applied, causing it to stretch beyond its capacity or tear completely.
Sports-Related Injuries
Many ACL tears occur in sports that involve quick changes in direction, sudden stops, or pivoting. These movements can put a significant amount of stress on the knee joint and the ACL.
Non-Contact vs. Contact Injuries
ACL tears can happen without direct contact (e.g., from an awkward landing) or as a result of contact (e.g., a tackle in football).
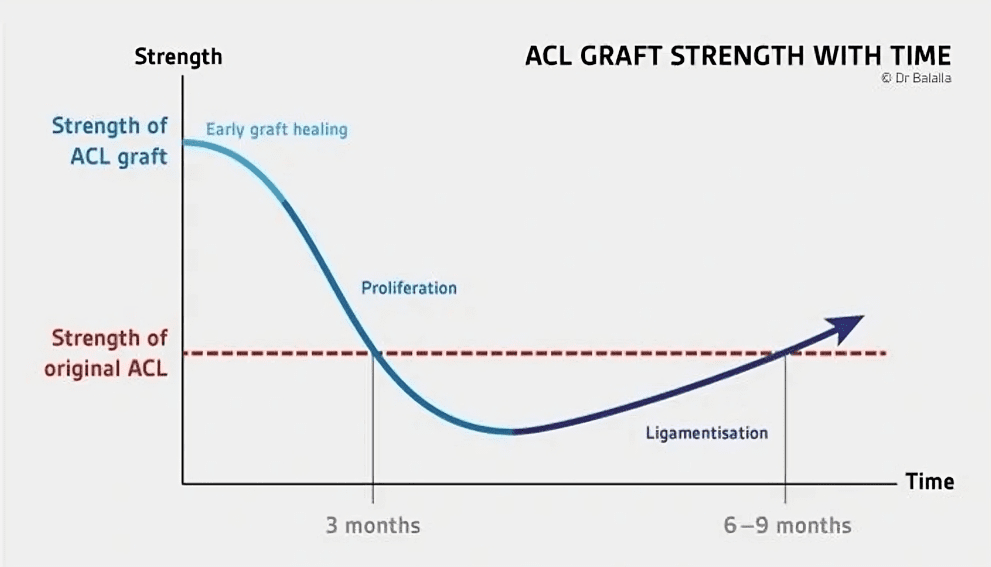
Recovery From an ACL Tear
Recovery from an ACL tear typically takes 6 to 12 months, and a full return to sports or high-impact activities might take longer, potentially up to a year. The duration varies based on the severity of the injury, whether surgery is needed, and the individual's recovery progress.
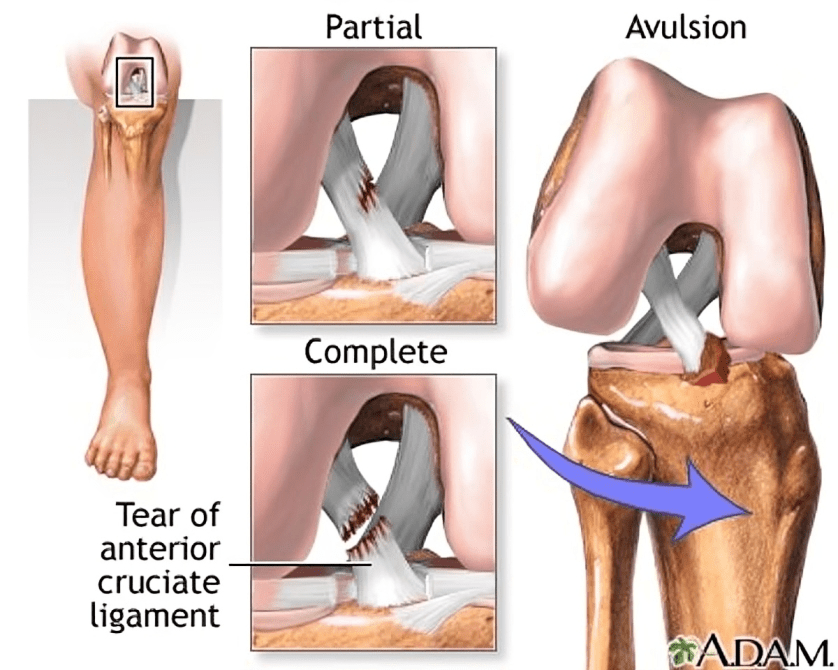
ACL Grades
ACL tears are graded on a scale of 1 to 3:
Detailed Breakdown of ACL Grades
Grade 1: Recovery
Recovery from a Grade 1 ACL tear, a mild sprain, typically involves a short recovery period and can be managed with the R.I.C.E. protocol and physical therapy. Most patients can return to normal activities within a few weeks, with full recovery often taking 2 to 4 weeks. Nonsurgical treatment is usually recommended for Grade 1 tears.
Detailed Recovery Steps
Grade 2: Recovery
Recovery from a Grade 2 ACL tear can take 6 to 8 weeks and may involve surgery. Non-surgical recovery often involves physical therapy, while surgery might be needed for those with persistent instability.
Elaboration
Grade 3: Recovery From a Complete ACL Tear
Recovery from a Grade 3 ACL tear, a complete tear of the anterior cruciate ligament, involves a multi-stage rehabilitation process. It can take anywhere from 6 to 12 months or longer to return to pre-injury activity levels. Surgical reconstruction is often recommended, using grafts from the patellar tendon, quadriceps, or hamstrings.
Rehabilitation Stages
Initial Recovery (Weeks 1-6)
This stage focuses on managing pain and swelling while beginning to restore motion.
Mid-Recovery (Weeks 6-12)
In this phase, the focus shifts to building strength and improving balance.
Late Recovery (Months 3-6)
This stage prepares you for more demanding activities.
Return to Sport (Months 6-12)
This final phase involves returning to full activity.
Important Considerations
Fractures
A fracture is a medical term for a break, crack, or shattering of a bone. Fractures can range from a hairline crack to a complete break where the bone is in multiple pieces.
Types of Fractures
Fractures are classified by how the bone is broken:
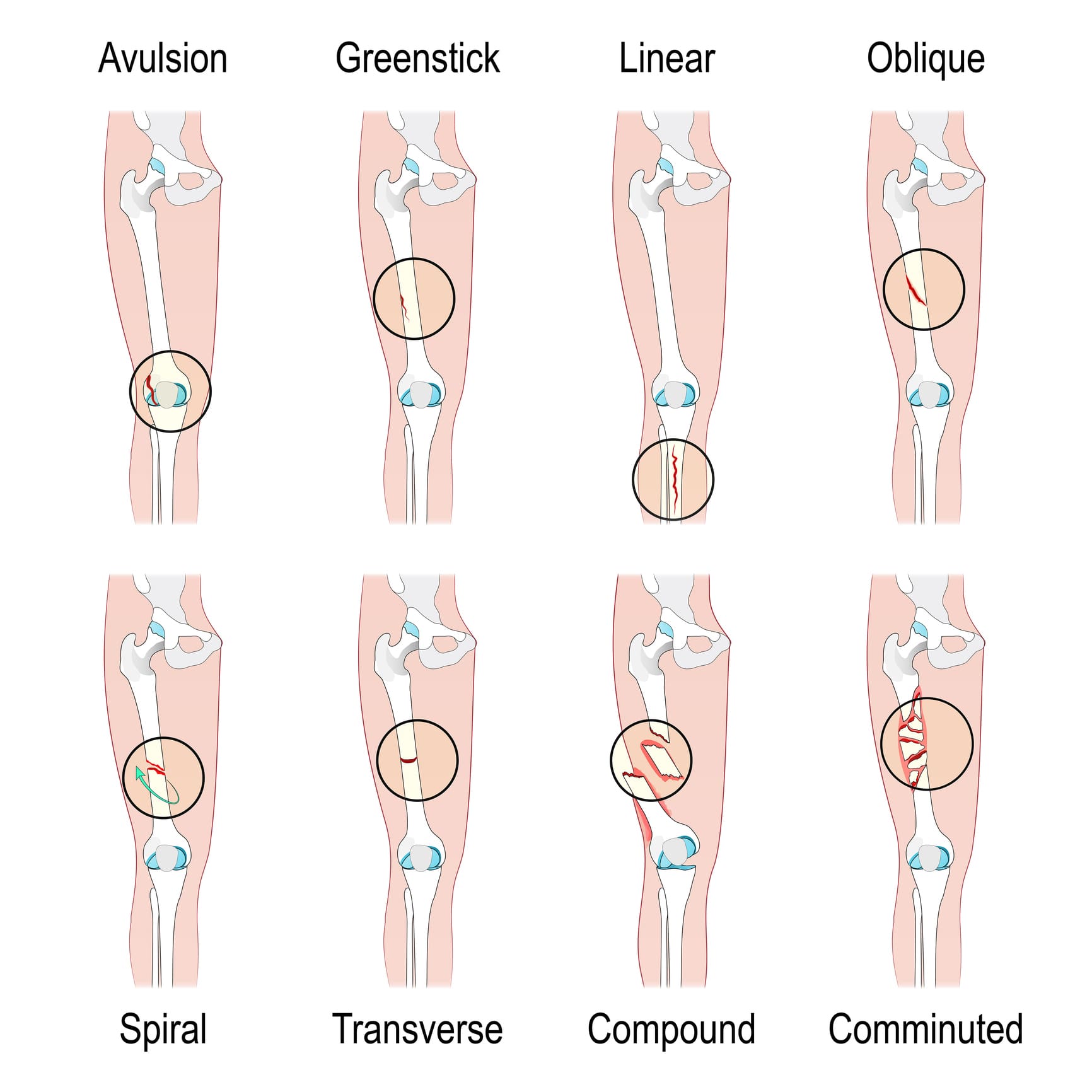
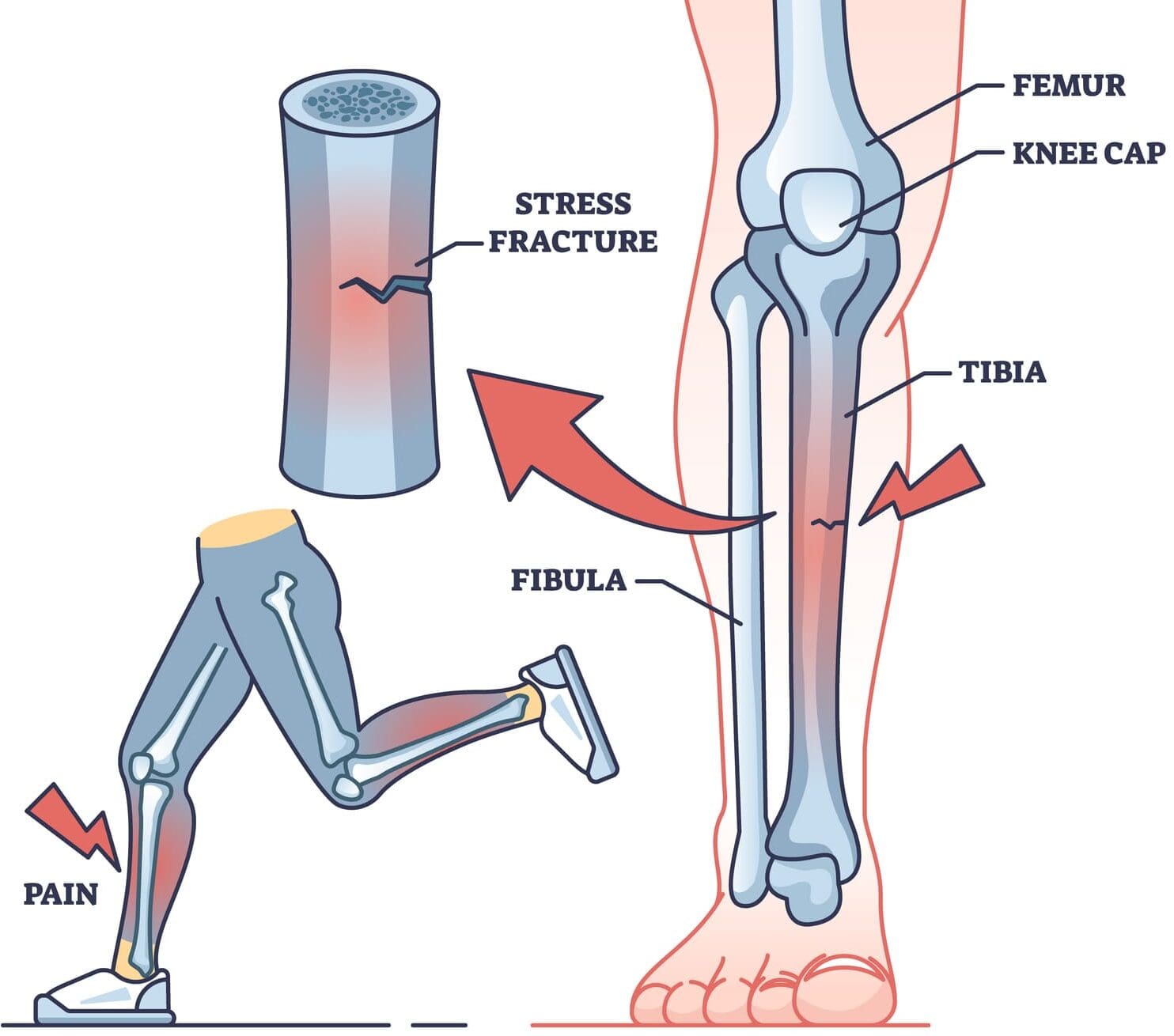
Causes of Fractures
Fracture Symptoms and Treatment
Fracture symptoms often include:
Treatment by Fracture Grade
These are minor cracks where the bone ends are still aligned, and the skin is intact. Examples include stress fractures and small toe or finger fractures.
- Treatment: Rest, immobilization with a splint or cast, ice, and elevation. Pain is managed with NSAIDs.
- Healing Time: 4–6 weeks, with physical therapy sometimes needed afterward.
Fracture Classification Systems
In addition to general grades, specific classification systems are used for different types of fractures.
Open Fracture Grading (Gustilo-Anderson System)
This system grades open fractures based on wound size and soft tissue damage.
Other Fracture Classifications
Concussions
A concussion is a mild traumatic brain injury (TBI) caused by a blow, jolt, or bump to the head, or a hit to the body that causes the brain to move rapidly inside the skull. This sudden movement can cause the brain to bounce or twist, leading to chemical changes and sometimes damage to brain cells.
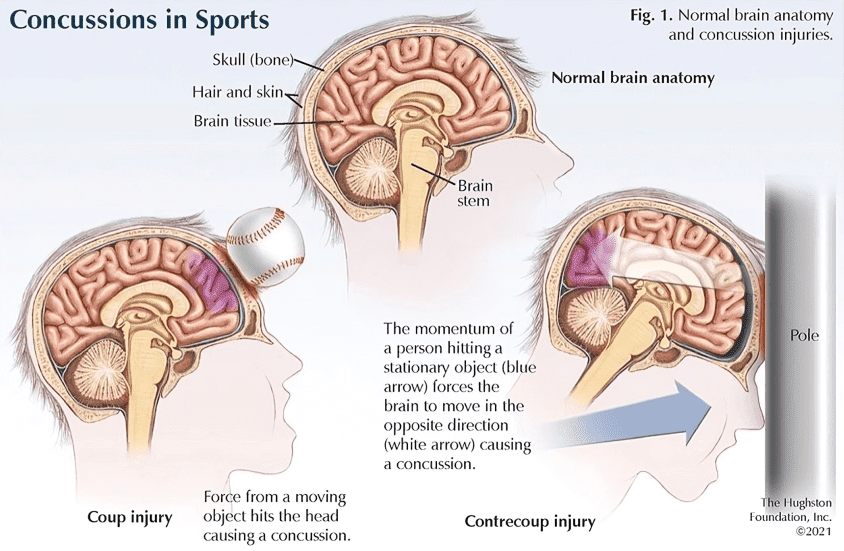
Causes of Concussions
Sports and Recreational Activities
This is one of the most common causes, especially among adolescents and young adults.
In many cases, concussions in sports go unreported because athletes fear being pulled from play.
Falls
Falls are the leading cause of concussions overall, especially among:
Falls account for about 50% of all TBI-related hospital visits in the U.S.
Motor Vehicle Accidents
Concussions frequently occur during:
Even minor "fender benders" can cause whiplash, resulting in a concussion if the brain is shaken inside the skull.
Assaults and Physical Violence
This includes:
Repeated head injuries from abuse can cause lasting neurological damage, especially in children.
Explosions and Blasts
This is particularly relevant to military personnel. Blast-related concussions can occur without a direct blow to the head, as the force of a shockwave can affect the brain by causing rapid pressure changes inside the skull. These are often called "invisible injuries" and may coexist with PTSD.
Workplace or Industrial Accidents
These are especially common in:
Occupational concussions are often underreported.
Workplace or Industrial Accidents
These are especially common in:
Occupational concussions are often underreported.
Repetitive Sub-Concussive Hits
Seen in athletes like football linemen or soccer players who head the ball. These impacts may not cause symptoms right away but can accumulate over time, increasing the risk of long-term brain disease like Chronic Traumatic Encephalopathy (CTE).
Concussion Grades and Treatment
Concussions are graded based on the severity of symptoms. The recovery and treatment plan for each grade focuses on rest and a gradual return to activity to prevent further injury.
This is the least severe type of concussion. There is no loss of consciousness, and symptoms like confusion, headaches, or dizziness last for less than 15 minutes.
- Treatment: Immediate removal from the activity and physical and cognitive rest for 24–48 hours. Avoid screens, studying, and exercise.
- Return to Activity: Return to school or work is recommended once symptoms are gone. A gradual, supervised return-to-play protocol is required before returning to sports.
- Recovery Time: Typically 7–10 days.
Concussion Symptoms
Concussion symptoms can be physical, cognitive, emotional, or related to sleep. It is important to be aware of all categories, as they can indicate a concussion even without a direct blow to the head.
Physical Symptoms
Cognitive Symptoms
Emotional Symptoms
Sleep Symptoms
Diagnosing a Concussion
Diagnosing a concussion involves a comprehensive clinical evaluation by a healthcare provider. Since most concussions do not appear on standard brain scans, the diagnosis is based on reported symptoms, a physical examination, and cognitive testing.
Diagnostic Steps
The first step is to gather detailed information about the injury and symptoms. This includes:
- How the injury occurred.
- Any loss of consciousness.
- Amnesia or memory gaps.
- Current symptoms like headache, dizziness, or confusion.
- Any history of previous concussions.
Doctors may use standardized symptom checklists like the Post-Concussion Symptom Scale (PCSS) to track the severity of symptoms and monitor recovery.
Red Flags That Require Immediate Attention
Seek immediate medical attention if you notice any of the following:
Meniscus Tear
What is a Meniscus?
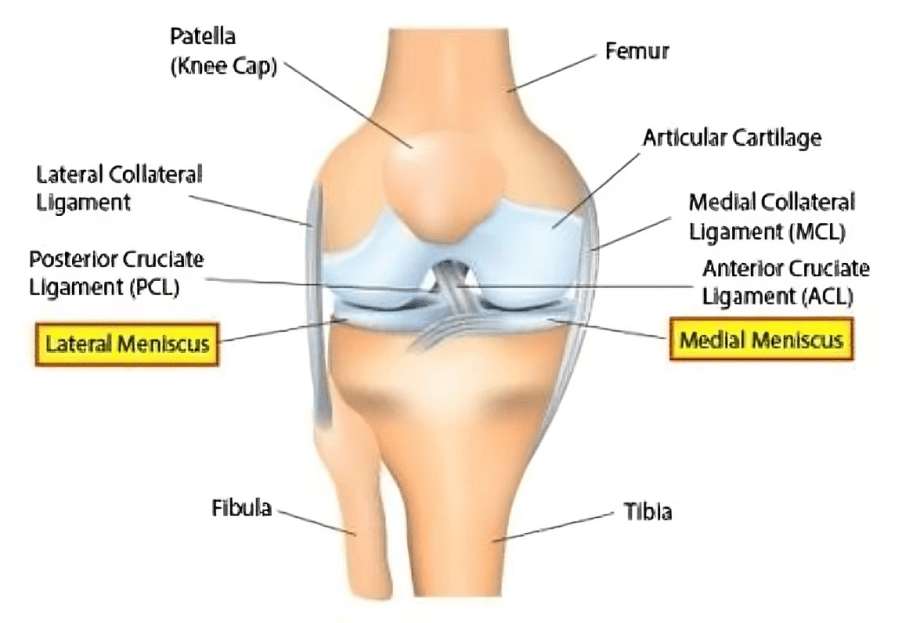
The meniscus is a C-shaped piece of cartilage in the knee joint that acts as a shock absorber between the thigh bone (femur) and the shin-bone (tibia).
You have two menisci in each knee:
They Help To
Causes of a Meniscus Tear
Acute (Traumatic) Tears
Common in young, active people. These tears are caused by:
Degenerative Tears
More common in older adults.
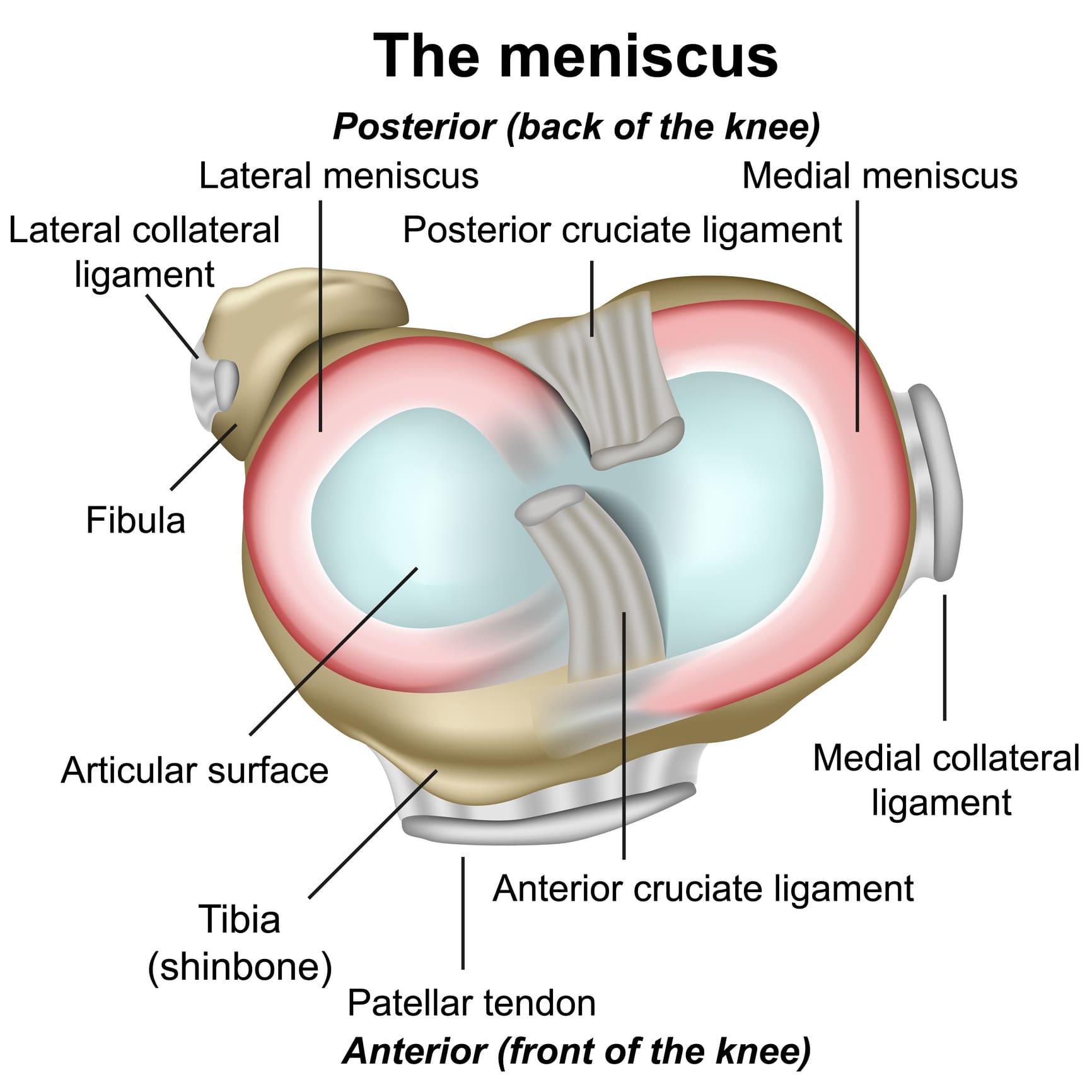
Types of Meniscus Tears
Different tear patterns affect treatment and healing:
Meniscus Tear Symptoms
The symptoms of a meniscus tear can vary depending on the location and severity of the injury. It is important to pay attention to these signs, as they may be mistaken for other knee injuries.
Common Symptoms
Popping Sensation
At the time of injury, you might feel or hear a pop, though it's often more subtle than with an ACL tear.
Pain
The pain is typically localized to the inner (medial) or outer (lateral) side of the knee, depending on which meniscus is torn. It may be mild at first, but it worsens with activities like twisting, squatting, or climbing stairs.
Swelling
Swelling usually develops more gradually than with an ACL tear, appearing several hours or even a day after the injury. Chronic or recurrent swelling can be a sign of a degenerative tear.
Stiffness and Reduced Range of Motion
The knee may feel stiff, especially after periods of inactivity. Bending and straightening the knee can become painful or limited.
Locking or Catching Sensation
A torn piece of the meniscus can get caught between the joint surfaces, causing the knee to lock or feel like it's catching during movement. You might also hear a click or snap.
Instability or "Giving Way"
While less common than with ACL tears, some people feel that their knee may give out, especially when walking on uneven surfaces or pivoting.
Difficulty Bearing Weight
Depending on the severity of the tear, walking or standing may be uncomfortable. Pain often increases with deep knee flexion, such as squatting or kneeling.
Symptoms of Chronic or Degenerative Tears

Meniscus Tear Treatment
Treatment for a meniscus tear depends on the tear's size, location, and the patient's age and activity level. Options range from non-surgical management to several types of surgery.
Non-Surgical Treatment
This approach is typically appropriate for small, stable tears, especially those in the outer "red" zone of the meniscus, where there is a good blood supply. It is also common for degenerative tears and for patients who are less active or have a higher surgical risk.
Components of Non-Surgical Management
R.I.C.E.
Rest the knee, Ice the area for 15–20 minutes several times a day, use a Compression bandage, and elevate the leg to reduce inflammation.
Medications
Over-the-counter NSAIDs (e.g., ibuprofen) can help relieve pain and inflammation.
Physical Therapy (PT)
A PT program focuses on regaining range of motion, strengthening muscles around the knee, and improving joint stability and balance. This typically lasts 4–8 weeks.
Bracing and Activity Modification
A knee brace may be used for support, and patients are advised to avoid activities like pivoting, sports, deep squatting, or repetitive stair climbing.
Surgical Treatment Options
Surgery may be required if the tear causes locking or instability, if conservative treatment fails, or if the patient is young and active.
This is the most common surgical procedure for meniscus tears.
- Procedure: The torn or damaged part of the meniscus is trimmed and removed using an arthroscope (a small camera).
- Indicated for: Tears in the "white-white zone" with poor blood supply, as well as complex or degenerative tears that cannot be repaired.
- Pros: Short recovery time (3–6 weeks) and is minimally invasive.
- Cons: The loss of meniscus tissue can increase the risk of developing osteoarthritis later in life.
Share Your Ideas
Have suggestions for other injuries? Connect with us.

